
Women’s Therapy in Calgary
Women’s Health
Therapy for women navigating identity, hormones, motherhood, medical trauma, pregnancy loss, and the cumulative weight of holding too much.

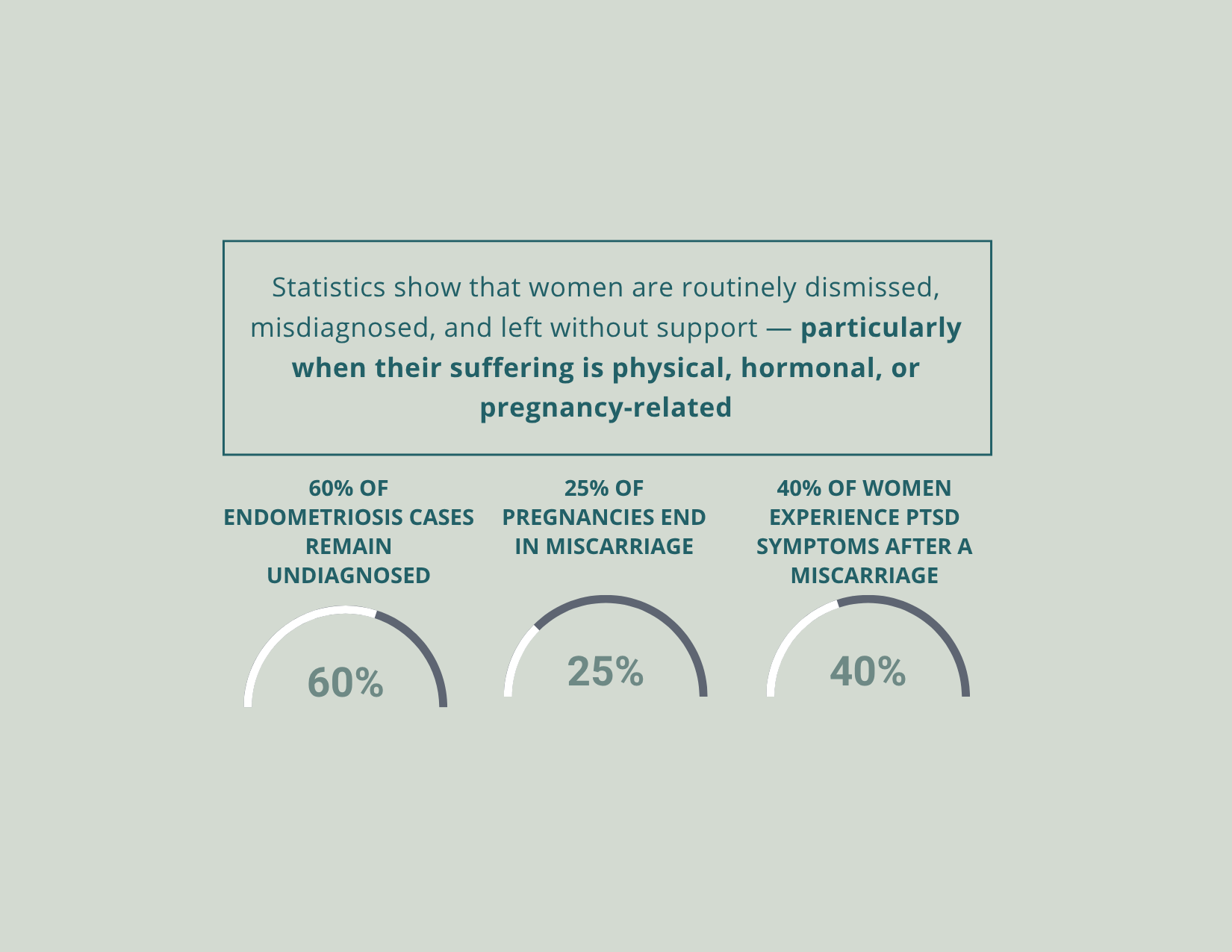
Sources: Yale School of Medicine, Public Health Agency of Canada, AMA
The Reality for Many Women.
You might feel like:
You're holding too much: parenting, work, the household, the relationships, the emotional weather of everyone around you
You're physically exhausted, but rest doesn't seem to fix it
You've been to doctors about the pain, the fatigue, the cycle, the symptoms, and walked away feeling unheard
Your hormones are shifting in ways no one prepared you for, and the language for it doesn't quite exist yet
You feel disconnected from your body, your partner, or yourself, in ways that have crept up slowly
You're carrying grief from a pregnancy loss, a fertility journey, or a version of motherhood that didn't unfold the way you thought it would
You've spent years being capable, and you're not sure who you are when the capacity finally runs out
You've tried therapy before, and it didn't quite reach what you actually needed help with
How Does Therapy Help Women?
Therapy at Carbon isn't just about coping skills or thought patterns. For most women who come to us, the work is bigger than that. It's about being heard, processing what hasn't been processed, making sense of what's been carried, and being seen accurately, including the parts of the experience that are physical, hormonal, or relational, not just emotional.
What this can look like:
Space to say what you've been holding without managing how it lands
Trauma processing for medical experiences, pregnancy loss, or relationships that left a mark
Working through the cumulative cost of being the one who holds everything
Reconnecting with your body, including the parts you've stopped trusting
Navigating identity shifts through motherhood, perimenopause, illness, or career change
Learning to receive support without feeling like a burden
Rebuilding the capacity to want things, ask for things, and trust your own knowing
For Women Living with Endometriosis, Chronic Pain, or Medical Trauma
Endometriosis is one of the most under-recognized conditions in women's health. The average woman waits years for a diagnosis. By the time she gets one, she's usually been told the pain is in her head, that she's anxious, that she's exaggerating, that nothing is wrong. The mental health consequences of being chronically dismissed by the medical system are real and largely unaddressed in standard therapy.
Therapy can be helpful if you're noticing:
Years of pain or symptoms that have been minimized or misdiagnosed
The mental health toll of medical appointments that didn't take you seriously
Anxiety, depression, or trauma symptoms that surfaced alongside chronic illness
The grief of a body that hasn't worked the way you wanted it to
Difficulty trusting medical providers, including male providers
The exhaustion of having to advocate for yourself in every appointment
Feeling alone in what you've been navigating
Jeremy Fonteyne, Registered Provisional Psychologist
Jeremy works specifically with women navigating endometriosis, chronic pain, hormonal conditions, and the medical trauma that often comes with them. Sessions focus on processing what hasn't been processed, working with the grief and anger that often accompany chronic illness, and building back the trust that's been worn down over years of dismissal.
For women who haven't always had positive experiences with male providers, Jeremy is also intentional about offering a steady, secure presence. A place where you don't have to brace, defend, or explain yourself before being believed. Many women find this aspect of the work meaningful in its own right.
Looking to Connect?
Whether you want to start therapy or support our community work, feel free to connect for more information.
For Women Navigating Pregnancy Loss, Fertility, and Reproductive Grief
One in four pregnancies ends in miscarriage. The mental health impact is substantial, and it often goes unmet. Most women who experience pregnancy loss receive minimal aftercare, are told some version of "it's common" or "you can try again," and are left to process the grief privately. The same is often true for fertility loss, recurrent loss, ectopic pregnancy, and the version of motherhood that didn't arrive on the timeline you expected.
This is grief, and it deserves real space.
Therapy can be helpful if you're navigating:
Recent or accumulated pregnancy loss
Recurrent miscarriage and the anxiety that builds with each subsequent pregnancy
Fertility struggles or the long, depleting process of trying to conceive
The ambiguous grief of bodies that haven't done what you needed them to do
Pregnancy after loss and the difficulty of trusting anything in your body again
The disenfranchised grief that pregnancy loss often produces. The kind no one knows how to acknowledge
Postpartum experiences that didn't go the way you expected
Finding the Right Fit.
Some women want a more direct, practical approach. Others want to do deeper trauma processing. Others want a steady, embodied space to make sense of what they've been carrying. We have therapists who work in all of these ways so that you can find someone who fits what you actually need.
The goal isn't to fix you. It's to help you make sense of what you've been holding, process what hasn't had space to be processed, and feel met in your full experience, including the embodied, hormonal, and medical dimensions that most therapy doesn't address.
The therapists on our women's health team work with EMDR, Internal Family Systems (IFS), Acceptance and Commitment Therapy (ACT), Emotion-Focused Therapy (EFT), narrative therapy, somatic and nervous-system-based approaches, and other evidence-based modalities, depending on what you need.
Why Many Women Don’t Seek Support.
For a lot of women, therapy is something they've considered for years before actually booking. They've recommended it to friends. They've made it possible for their partners or kids to access support. They've held space for everyone else. By the time they finally come for themselves, they're often well past the point where the work would have been easier.
You may have learned, somewhere along the way, that your needs come last. That asking for help means you're failing at the thing you were supposed to be naturally good at. That being capable means handling things on your own.
You may also have had previous experiences, with therapists, with doctors, with people you tried to be honest with, that didn't quite land. Where what you said wasn't fully heard, or what you felt wasn't taken seriously, or you walked away feeling like you should have been further along than you were.
FAQ
-
Is it normal to feel exhausted, disconnected, or numb even when life looks fine on paper?
Yes. For many women, this is one of the most common experiences that brings them to therapy. The cumulative cost of holding too much, for too long, often shows up as flatness, low-grade depression, or a sense of being far away from yourself — even when externally everything looks okay.
-
Do you work with women navigating chronic illness or medical trauma?
Yes. Several of our therapists, particularly Jeremy, work in this area. Therapy with us takes the embodied and medical dimensions of women's health seriously. We don't separate mental health from what's happening in your body.
-
I've had a pregnancy loss. Can therapy help, even if it was a while ago?
Yes. Pregnancy loss often goes underprocessed at the time it happens, and the grief can resurface years later, sometimes during a subsequent pregnancy, sometimes during a transition, sometimes in ways that aren't immediately recognizable as related. There's no expiration date on this kind of grief. We work with women navigating recent and long-held losses.
-
How can a male therapist help with women's health concerns?
A good therapist's effectiveness isn't determined by gender. What matters more is whether they're attuned, skilled, and able to hold the kind of work you need to do. For women navigating medical trauma in particular, working with a male therapist who is steady, attentive, and respectful can be its own form of repair, a chance to experience being taken seriously by a man in a clinical context, when other men in clinical contexts haven't always offered that. Some women prefer a female therapist regardless, and that's valid too. Both options are available.
-
Can I come to therapy if I'm not in crisis?
Yes. Most of the women we work with aren't in acute crisis. They're functioning, often well, and they're tired of doing it without support. You don't need to wait until things have fallen apart to ask for help.
-
I don't know what's wrong, just that something is. Is therapy still useful?
Yes. A lot of women come in without being able to name what's happening — just a sense that something has shifted, or that they're not okay, or that they're carrying more than they should be. Part of the early work is making sense of what's actually going on. You don't have to arrive with a diagnosis or a clear story.

